Personalized Precision Medicine


We are all unique. Our nucleotide pairs, beliefs, memories, and life experiences are singular and inimitable. Most people I know take comfort in the idea that the mold broke after making them. Our oneness should be very material in administrating healthcare and tending to our medical needs. Unfortunately, it seems all that uniqueness has been broadly disregarded for decades. A few basic traits categorize us, such as gender and age, which have significantly influenced how diagnostics, devices, medication, and health sciences have evolved.
Most medical treatments are designed for the average patient, for the average person, in other words, taking the “one size fits all” kind of approach. We’ve been doing this in medicine for decades, really centuries, for medical devices as well as drugs. The result is that some products might be successful in some patients, but for other patients, not so much, and for the third set of patients, those medical devices and drugs could be flat-out dangerous.
Mike Drues, president of Vascular Sciences. Taken from Personalized Healthcare—Mike on Medtech

The diagnostic procedure or remedy with the highest efficacy for the average patient becomes a defacto “gold standard” without taking into account more precise data. One size fits all means critical indicators derived from our personal needs are ignored.
The one size fits all approach works… for a car
The one size fits all approach mimics the relationship between a mechanic and a car. Let’s classify visits to your local garage into three categories: regularly scheduled maintenance, repair work due to an accident, or a known/unknown issue affecting the car’s performance. In each instance, the mechanic would follow a standard procedure to check, replace or troubleshoot the problem.
This approach ensures consistency. Repeating the most efficient and cost-effective steps for the same issue delivers the desired result with minimal chances of error, provided you have a good and honest mechanic. And this makes sense because you wouldn’t tell each Toyota Camry it is unique compared to all the other Toyota Camrys out there.
Humans are admittedly much more complex than cars. We collectively share many similar traits. However, our uniqueness influences our healthcare and medical needs depending on the procedure or diagnosis. How does impersonalized medicine fail us?
Treatment efficacy rate is not as high as you think
If you had to guess, how often are the medications and treatments received effective? More than 50%? 80%? It is hard to find a consensus on this metric. Realistically, without delving into the specifics of each treatment, it would be hard to produce a single number to represent a global average. That hasn’t stopped others from trying. There are wildly disputed figures, putting average effectiveness as low as 30%.
The number needed to treat (NNT) … is the number of patients who need to be treated for one patient to benefit. For example, consider a drug that decreases mortality of a certain disease from 10% to 5%, an absolute risk reduction of 5% (1 in 20). That means that of 100 patients, 90 would live even without treatment, and thus would not benefit from the drug. Also, 5 of the 100 patients will die even though they take the drug and thus also do not benefit. Only 5 of the 100 patients (1 in 20) benefit from taking the drug; thus, 20 need to be treated for 1 to benefit, and the NNT is 20
Taken from Drug Efficacy and Safety – Clinical Pharmacology – Merck Manuals Professional Edition
Let’s use the NNT data for an ischemic stroke treatment as an example, taken from Tissue Plasminogen Activator (tPA) For Acute Ischemic Stroke. The effectiveness is time-dependant:
| Time to administer drug | NNT |
|---|---|
| 0 to 3 hours from onset | 10 |
| 3 to 4.5 hours from onset | 19 |
| 4.5 to 6 hours from onset | 50 |
Delayed treatment is critical in diminishing the effectiveness, yet even when administered in a timely fashion, only 10% of patients benefitted from the treatment. 90% were ineffective. There is a staggering savings of costly drugs and human resources to be had if a better approach could be employed.
Diagnosis errors occur frequently
It is likely that most of us will experience at least one diagnostic error in our lifetimes, sometimes with devastating consequences.
Improving Diagnosis in Health Care
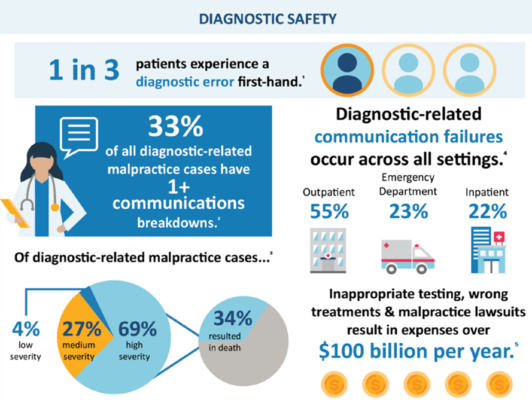
The wrong diagnosis prolongs the suffering and illness of the patient and lowers the chance of a complete recovery. The phrase “time is muscle” was introduced by Eugene Braunwald, meaning the more extended a heart-related issue goes untreated, the more damage endured. There are irreversible and often fatal consequences when precious time is lost in an emergency.
While many factors contribute to diagnostic errors, the question is, by using the average patient approach, are we increasing that probability? Is there critical information that a precision medicine approach includes which would change the diagnosis? The short answer is yes; more personalized data decreases the chances of misdiagnosis. Literature on this topic tends to focus on data management; existing patient records which are not easily sharable due to legislative or logistical barriers.
Let’s look beyond a specific patient’s immediate needs and take a more systematic view, focusing on diagnostic procedures. It is possible to create a digital twin of the patient for use in CAE-type simulations for diagnosis. However, it is not commonly employed, even if the technology is ripe for exploitation. Simulation is no doubt an essential asset to the personalized precision medicine approach.
Under the virtual knife
Once a diagnosis is made, several treatment options will likely be possible. Which is the best course of action becomes a question of probabilities. Their validity depends on medical experience and available information, all most likely based on the average patient.
It is usually risky or impossible to start with one invasive intervention and decide to switch and apply a second approach instead should the first prove wrong. It is difficult to compare different treatment options’ predicted net benefit or validity when the expected outcome is based on the average patient fallacy.
Performing a “what-if” analysis on a living, breathing person is impossible. Yet digitally exploring different treatment options causes no harm and might provide better insights. Personalized precise medicine, amongst many other goals, aims to reduce the chances of wrong procedures being performed by better understanding the problem and making a more accurate prediction of the expected outcome. While this field is still emerging, simulation can help personalize the devices and treatments to accommodate different morphologies.
Simulating airflow to assist in diagnosis and intervention planning
Computational Fluid Dynamics (CFD) simulation can be essential in diagnosis and intervention planning in respiratory medicine. CFD simulations allow the airway to be assessed and breathing quantified in a way not previously achievable, leading to opportunities to improve patient care.
Dr. Alistair Bates, Cincinnati Children’s Hospital Medical Center, believes CFD simulations will play a significant role in the future of respiratory medicine. In this on-demand webinar, Dr. Bates uses the example of premature newborn babies in respiratory distress. First, he demonstrates how CFD simulations with Simcenter can quantify the effect of diseases such as tracheal collapse. Then, he explains how this information informs clinical decision-making. His approach is to create realistic airway motion in the simulation, which allows diseases in which the airway collapses to be studied.
Personalized 3-D printing
Additive manufacturing is another emerging technology that plays a role in the personalized precision medicine approach. Companies such as LimaCorporate and Unlimited Tomorrow are disrupting their respective industries with 3D-printed implants and prostheses – read Engineering Enhanced Humans for more details on their stories.
Overcoming the barriers to innovation with next-generation medical device design solutions is another great on-demand webinar on this topic. The focus is on accelerating product development using additive manufacturing solutions to realize new medical device designs.
Above average results
We are at the cusp of realizing what personalized precision medicine can offer. I’ve only highlighted a few examples. Practitioners will continue researching and finding novel ways to incorporate simulation and digital evidence into their diagnosis and decision-making. You might not be precisely like the average patient. With Simcenter, the average patient doesn’t have to be you to make your next visit to the doctor a bit more personal.